The Answer to the Adherence Problem at Community Health Centers
Patient medication compliance is a major problem in the United States.
In fact, medication adherence is such a big issue that it makes up 13% (or $290 billion) of all healthcare spending annually. Patients across the country struggle with adherence, but the problem is especially prevalent among the uninsured — and underinsured — patient population.
Fortunately, new pharmacy technology can help pharmacists improve medication adherence with patients, some of which are considered high-risk, at community health centers (CHCs) across the country.
Telepharmacy is here, and it’s helping pharmacists solve the adherence problem at community health centers.
Defining the adherence problem
In order to understand how big of an impact telepharmacy can have, let’s first make sure we comprehend the enormity of this issue.
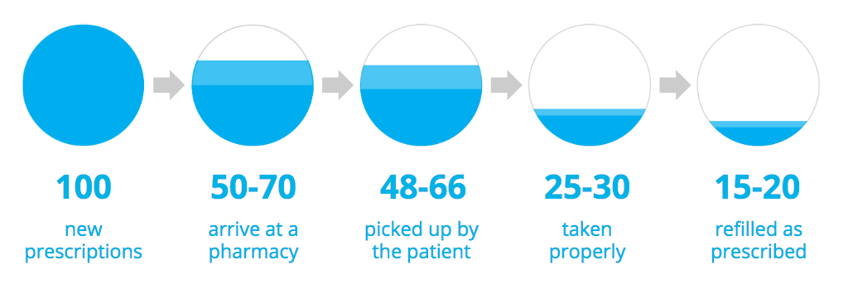
Source: IMS Health Data, March 2011
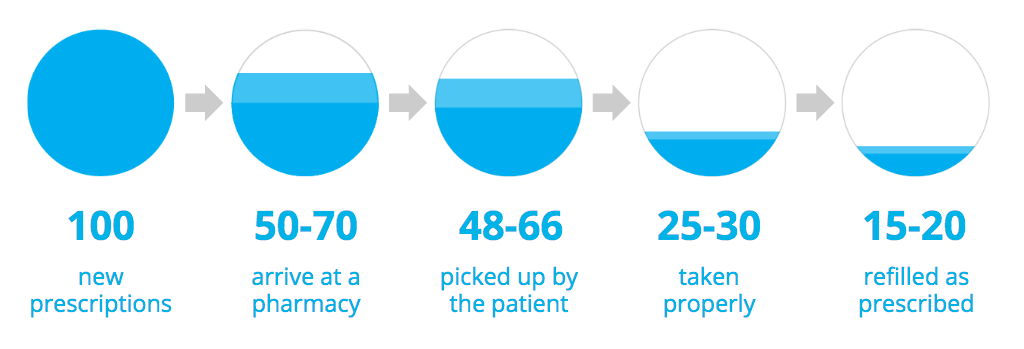
The above graphic is known as “the leaky bucket.” According to an IMS Health data study, out of every 100 new prescriptions, only 50-70 arrive at a pharmacy. Only 48-66 of those 100 prescriptions are picked up by the patient, and only 25-30 of those prescriptions are taken properly. On average, 15-20 of those 100 new prescriptions are refilled as prescribed.
Pharmacists can help in every step of the process. Convenience, for example, plays a big role in whether or not a prescription actually arrives at a pharmacy. According to a Kaiser Permanente study, 95% of patients filled their initial prescription when offered the option to do so at the doctor’s office. If we can improve our chances at the top of the funnel, the trickle-down effect will certainly help improve adherence rates.
A solution for community health centers
UW Health, one of our customers, started exploring partnership opportunities with local community health centers. Joe Cesarz, Pharm.D., Manager, Ambulatory Pharmacy Services, wanted to set up a partnership and provide pharmaceutical care services to Access Community Health Center, a local health clinic.
“When we were evaluating this location (Joyce & Marshall Erdman Clinic), the struggle was the volume didn’t really justify having a full-fledged pharmacy with a pharmacist on-site,” Joe said, discussing the logistics. “At that time, we started exploring different options to at least provide some dispensing services to the clinic at a lower cost, or at least more efficiently.”
Joe and his team discovered telepharmacy and TelePharm’s software platform and wanted to implement the solution to open a remote-dispensing site.
“One of our strategies was where can we offer dispensing services where the volume doesn’t necessarily justify it” he said, discussing the strategy and level of service when it comes to telepharmacy. “The second strategy was how can we use TelePharm to decouple the pharmacist from the dispensing and product process in the pharmacy and use those resources more in the clinic. If we can provide the same level of service that a patient would receive at a pharmacy when it comes to product verification, patient safety, as well as pharmacist consult and medication education and training for patients, if we can achieve that in my mind that’s success.”
Making adherence easy for patients
UW Health opened their remote-dispensing site at the Access Community Health Center roughly two years ago and have seen the prescription count grow steadily over time. Nora Groeschel, Pharm.D., Pharmacy Manager, thinks this the telepharmacy model is good for patient adherence because it provides a one-stop shop for patients.
“I feel like so many patients that we individually deal with are in the door very infrequently and you have a one touch opportunity while they are here,” she said. “We are going to see you for this and we are going to order your medications, and given that if you send them to a different, outside pharmacy and say, “Oh, just go pick them up,” there’s issues and chances are they might not go pick them up at all or they show up and there’s issues and they can’t be dealt with.”
With increased access to the pharmacist comes better patient education which translates to more patients filling prescriptions and taking their medication as prescribed. Increasing access to a pharmacist can help elevate the not-so-great numbers highlighted in the leaky bucket.
“When you have a remote-dispense site in the clinic, the patient comes in and we try and do everything all at once and if there’s problems we try to address them right away.”
Patients (and pharmacists) take a liking to new technology
Melissa Ngo, Pharm.D., Pharmacy Manager has had a passenger seat in watching UW Health’s telepharmacy program evolve from a longshot idea to a successful way of delivering high-quality pharmacy care services to patients. But that didn’t come without reservations.
“When the technology first came across I was a little hesitant because being an old-school pharmacist, I was so used to that pharmacist-patient interaction and I felt that you developed relationships with that in-person interaction,” she said, on the topic of video counseling patients. “Once I saw the technology and we started using it, that face-to-face interaction still occurs, the fact that we can use technology and that patient can see the pharmacist they are talking to and have a conversation, the display screen is pretty big and the vocalization both ways is very clear. We have the same group of pharmacists counseling for our remote dispense sites so the patients are still seeing that same face every time they come in.”
Melissa said she was pleasantly surprised with how well telepharmacy software works, and the patients have the same sentiment.
“It’s been phenomenal! I will tell you the patients have complimented the technology and feel that they are still getting exactly what they need.”
Interested in helping patients at your Federally Qualified Health Center (FQHC) or Community Health Center (CHC) be more adherent to their medication(s)? Contact us to learn if telepharmacy is right for your organization.



